 Tomorrow is World Asthma Day.
Tomorrow is World Asthma Day.
We would be remiss if we didn't discuss the importance of recognizing asthma and its negative impacts on sleep.
It's also important to know that asthma, especially nocturnal asthma, has the potential to both cause and aggravate sleep apnea.
What is asthma?
Asthma is a chronic disease of the lungs and airways. It occurs when the airways become inflamed and constricted, making it difficult to breathe. During the day, the disease expresses itself as coughing, wheezing, shortness of breath, tightening of the chest, and panic or anxiety related to not being able to breathe.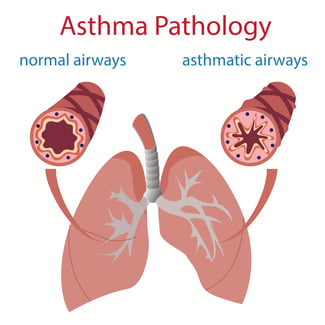
The National Heart, Lung, and Blood Institute estimates that 20 million Americans suffer from asthma. More children than adults tend to have asthma.
Asthma used to be considered a part of the spectrum of lung disorders known as chronic obstructive pulmonary disease (COPD).
It is no longer considered necessary to have asthma in order to be diagnosed with COPD (a combination of chronic bronchitis and emphysema).
However, asthma is still commonly experienced by people suffering from COPD, and both conditions may aggravate each other.
What is nocturnal asthma?
Episodes of asthma which occur at night and show a worsening of the disease are known collectively as nocturnal asthma.
People with nocturnal asthma often suffer from nighttime coughing, wheezing, and breathlessness that disturbs their sleep.
Nocturnal asthma is not common to all asthma sufferers, but it does indicate the presence of more severe disease and higher risks for mortality. For some people with asthma, it's their nocturnal asthma which troubles them most.
As many as 3 out of 4 asthmatics suffer disrupted sleep at least once a week due to nocturnal asthma, with 40 percent suffering from asthma symptoms every single night.
Nocturnal asthma and sleep apnea
Research shows that people with asthma are more likely to develop obstructive sleep apnea (OSA).
OSA is a serious sleep-breathing disorder in which mechanical obstruction of the airways during sleep causes repeated pauses in breathing. These pauses can greatly disrupt blood oxygen levels and lead to sleep fragmentation.
OSA and asthma have overlapping symptoms that can make each condition to differentiate from the other.
Some clinicians think the similarities are so strong between the two that nocturnal asthma should be considered a sleep-breathing disorder, as it has as serious an impact on sleep as sleep apnea.
Getting a differential diagnosis is critical;  some asthma therapies may, in fact, aggravate an underlying and undetected OSA condition.
some asthma therapies may, in fact, aggravate an underlying and undetected OSA condition.
People with either sleep apnea or asthma, who suspect they might have both, may request a referral to a sleep specialist for testing to rule the other condition in or out. This is useful for finding appropriate treatments for both conditions.
Symptoms of nocturnal asthma
These are similar to daytime symptoms except that they occur during sleep and can cause significant problems with getting enough sleep, such as
-
Coughing that disrupts sleep
-
Wheezing that disrupts sleep
-
Shortness of breath upon awakening
-
Chest tightness upon awakening
What causes nocturnal asthma?
There might be a circadian rhythm dysfunction that leads to nocturnal bouts of asthma symptoms, but researchers aren't certain and need to conduct more studies. Other more obvious causes include:

-
Exposure to triggers such as allergens, pollutants, viruses, foods, or strong odors
-
Chronic and undertreated sinus problems such as sinusitis and postnasal drip
-
Air conditioning that overcools the upper airway too quickly
-
The presence of GERD (gastroesophageal reflux disease, or acid reflux), which can occur in tandem with both OSA and nocturnal asthma
-
Certain medications that trigger asthma attacks, such as beta blockers for migraines and blood pressure, or anti-inflammatory drugs like aspirin and pain relievers
-
Increased upper airway resistance during sleep due to a sleep-breathing disorder
-
Other normal changes to the airway during sleep which are common in all people, but which show more adverse reactions in those with asthma
-
Delayed asthmatic response (in which an attack occurs 3 to 8 hours after exposure to the trigger)
 How to treat nocturnal asthma
How to treat nocturnal asthma
There's no cure for asthma, but it can be controlled by the following:
-
Maintenance medications to reduce swelling
-
Quick, temporary inhaler treatments for acute symptoms
-
Trigger avoidance to prevent attacks from happening (especially food allergens and dust mites)
-
Vigilant self-monitoring using a peak-flow meter to prepare for likely attacks
If you struggle to breathe at night, you may have nocturnal asthma. In fact, some people do not realize they have asthma at all until nighttime symptoms develop. It's very important to have these symptoms checked out by a physician. Most patients with nocturnal asthma meet diagnostic criteria for moderate or severe persistent asthma, which must be treated.

Untreated nocturnal asthma is dangerous, as it can lead to excessive daytime sleepiness, sleep deprivation, and the critical loss of important lung function.
In any case, having asthma at night is going to make you miserable, so don't delay in identifying and treating it.
Sources
Journal of Allergy and Clinical Immunology
Medscape Multispecialty
National Heart, Lung, and Blood Institute
National Jewish Health
National Sleep Foundation













Leave a comment