 Sleep apnea is the next most common sleep disorder after insomnia. It impacts at least 18 million Americans. It is estimated that 10 percent of the entire US adult population suffers from obstructive sleep apnea (OSA), its most prevalent form.
Sleep apnea is the next most common sleep disorder after insomnia. It impacts at least 18 million Americans. It is estimated that 10 percent of the entire US adult population suffers from obstructive sleep apnea (OSA), its most prevalent form.
However, anywhere between 40 and 80 percent of people with OSA are not even aware they have it. Or if they are, they choose not to be diagnosed or to be proactive about treating it.
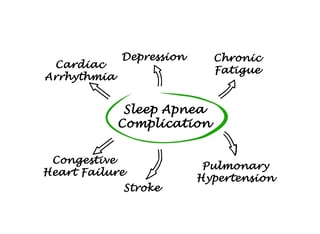
Untreated, undiagnosed sleep apnea risks the development of multiple chronic health problems as well as injuries, increased healthcare expenses, and quality of life issues, all which can be avoided.
The Dangers of Untreated Sleep Apnea
Chronic disease
The American Academy of Sleep Medicine (AASM) lists these negative long-term health consequences for someone with untreated sleep apnea:
-
High blood pressure
-
Heart disease (coronary artery disease, congestive heart failure, cardiac arrhythmia)
-
Stroke
-
Pre-diabetes and diabetes
-
Depression
 The AASM further explains that people with moderate to severe OSA are “four times more likely to die when the sleep disorder is left untreated in the long term.”
The AASM further explains that people with moderate to severe OSA are “four times more likely to die when the sleep disorder is left untreated in the long term.”
Other research shows additional problems independently linked with untreated sleep apnea consequences.
A study in the Journal of Clinical Sleep Medicine showed that cancer patients with untreated OSA were four times more likely to die than those without OSA or who were treating their OSA successfully.
Dr. Vishesh Kapur at the University of Washington led a team of researchers to discover a link between undiagnosed or untreated OSA and increased adverse outcomes for surgical patients. This is because patients with untreated OSA are in greater danger of respiratory failure while under general anesthesia.
Another study published in Thorax in 2015, of more than 3 millions veterans with OSA, concluded that without active treatment for their sleep apnea, they more likely suffered from chronic kidney disease.
The president of the AASM, Dr. Safwan Badr, sends out the message, loud and clear: "Obstructive sleep apnea is a chronic disease that can be destructive to your health."
Injury risks
If you have untreated OSA, you are likely sleep deprived. The frequent fragmenting of your sleep, night after night, is caused by sleep apnea's dysfunctional breathing patterns.
This means you aren’t getting the healing, restorative rest your body and brain need to function optimally during the day. Injury is a major outcome of sleep deprivation.
People with untreated OSA are 3 times more likely to suffer from workplace accidents. The ratio jumps dramatically in the case of car crashes. Undiagnosed OSA leads to a 15 to 20 percent increase in the risk for sleep-related traffic accidents!
Accidents while on the job, or during operation of a motor vehicle, are frequently due to sleep deprivation caused by untreated OSA. This leads to impaired vigilance, a decreased ability to adequately perform daily tasks, and greater chance for making critical decision-making errors.
The high cost of untreated sleep apnea
Medical expenditures
A study led by Sassani in 2004 estimated that over 800,000 automobile accidents in one year could be attributed to OSA, with nearly 1500 fatalities and $16 billion in costs as a result.
However, if the OSA was treated, they factored in the cost of CPAP therapy (as dollars saved) and concluded that half a million of those accidents could be prevented, reducing lives lost to less than 500, and reducing healthcare costs by over $11 billion.
In the UW study, Dr. Kapur and his team found that the mean annual healthcare costs for a person with undiagnosed, untreated OSA (prior to diagnosis) were nearly twice those of someone without OSA, even when adjusted for age, gender, and body mass index.
The economic burden is not only felt by insurance companies, Medicare providers, and healthcare professionals. The UW study showed that people with OSA are ten times more likely to file for workplace disability. This drives up an employer's healthcare costs and reduces overall productivity.
People with untreated OSA aren’t off the hook, either. They spend more time and money on healthcare than their healthy cohorts, expenses that could be reduced if they treated their OSA. At least one study has shown that patients with OSA plus severe heart and lung disease significantly reduced their total healthcare costs after using continuous positive airway pressure (CPAP) therapy to treat their OSA.
Investing in a sleep study, ge tting a diagnosis of OSA, and applying PAP therapy could be one of the best investments you ever make in your health. Treating OSA seems to help reduce risk factors or improve symptoms for many other chronic health conditions you might also suffer from.
tting a diagnosis of OSA, and applying PAP therapy could be one of the best investments you ever make in your health. Treating OSA seems to help reduce risk factors or improve symptoms for many other chronic health conditions you might also suffer from.
Quality of Life
Untreated OSA makes it hard to get out of bed. Morning grogginess, daytime sleepiness, hypersensitivity, cognitive fogginess, and irritability are all common adverse effects for people with untreated OSA.
Without treating sleep apnea, these markers of sleep deprivation quickly become the norm, leaving people unhappy and lacking in the energy and focus necessary to lead full, meaningful lives.
OSA can lead to job dissatisfaction, burnout, and relationship problems as well.
If you've already been diagnosed...
Chances are, you have given up on therapy because you found it uncomfortable or undesirable. You may have been diagnosed several years ago, and stuck with PAP therapy for a while, and felt better, so you stopped using it. Or you might have been more recently diagnosed but, because of delays in insurance authorization or a fear of using the equipment, you lost your motivation to use it.
Here’s what you can do if you want to treat your OSA but dread the thought of using PAP.
-
Try a different mask. Sometimes patients are given the wrong mask style or size. Keep trying! You’d be surprised at the comfort of a well-fitting mask.
-
Ask about bilevel PAP. This form of therapy has customizable settings to improve the comfort of PAP delivery.
-
If you have an older machine, replace it. Newer machines are quieter, more sophisticated, and include heated humidification, not often found on dated equipment.
-
Join a support group. A.W.A.K.E. has chapters all around the country with gather together people with sleep apnea to share tips, encouragement and success stories. Find groups in KS.
-
If anxiety is your issue, learn breathing strategies. These can help both relieve your stress and improve your experience with PAP. It can take some practice to overcome claustrophobic feelings, but many people have overcome their fear of masks to become CPAP “super users.” You could become one of them, too!
-
Inquire into dental sleep medicine. For some patients, an oral appliance can be effective for treating OSA. For severe OSA patients, a combination of both an oral device and a form of PAP may work as well.
-
Look into procedures. For people with abnormalities in their nasal or oral cavities, a surgical procedure can provide relief for sleep breathing problems. PAP is not a good option for someone with a deviated septum, for instance. A surgical correction may be an appropriate choice.
-
Consider neurostimulation. These new devices are implanted into the chest like pacemakers; they send brief electrical pulses to the upper airway to maintain adequate space and tissue tone for better breathing all night long.
Whatever you do, be aware that CPAP is not your only option, but there is a price you pay if you forego treatment of your OSA.
If you suspect you might have sleep apnea...
Consider whether you might present with the symptoms of sleep apnea. You might: 
-
Snore regularly, and often quite loudly
-
Suffer from daytime drowsiness and fatigue
-
Wake up all night long for no clear reason, or to use the bathroom several times
-
Awaken in the morning, short of breath, or with a dry mouth, sore throat, or headache
-
Feel uncharacteristically crabby during the day
-
Struggle with attention and focus
-
Have nightmares in which you feel you are drowning
-
Be previously diagnosed with resistant hypertension
If any or all of these things sound familiar to you, a trip to your primary care physician with a sleep study request should be your next move. Dr. Badr of the AASM concurs, giving this advice: “People with symptoms of sleep apnea… should see a board certified sleep medicine physician for a comprehensive sleep evaluation."
Once evaluated and diagnosed, the good news is this: OSA is treatable, with multiple options for doing so. Give it your best shot—try all the alternatives available to you to get the best therapy possible.
Whatever else you do, take action now! You don’t want to be one of the many walking around with an untreated case of sleep apnea (and all its related health problems).













Leave a comment