 Difference Between APAP, BiPAP, CPAP, and ASV
Difference Between APAP, BiPAP, CPAP, and ASV
When you've been diagnosed with sleep apnea, your first therapy option is, typically, some form of positive airway pressure (PAP) medical device.
These all fall under the umbrella of what is known as noninvasive ventilation (NIV).
Which device you are prescribed depends upon what kind of sleep apnea you have—obstructive sleep apnea (OSA), central sleep apnea (CSA), or a combination of the two—as well as how severe you are, and what other kinds of health conditions influence your sleep-breathing problems at night. It may also depend upon how well you respond to any given therapy.
What are the different styles of NIV therapy available? Let's break them out.
What is CPAP?
CPAP stands for continuous positive airway pressure. It's the most commonly used therapy to treat sleep apnea. It involves a motorized device which pressurizes air it draws from the room. Once pressurized, it delivers the air through tubing connected to a mask you wear on your face as you sleep.
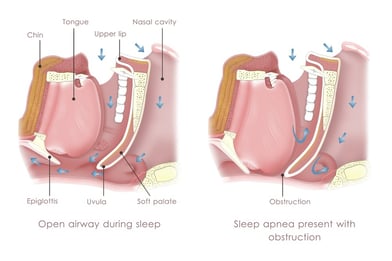 How does CPAP work?
How does CPAP work?
CPAP delivers a single continuous stream of pressurized air to help keep your upper airway from collapsing while you sleep.
(If you're not sure why you're airway might collapse during sleep, check out this post on sleep apnea.)
PAP is often described as a kind of mechanical airway "splint."
Who uses CPAP?
People with all severities of OSA use CPAP. The more severe one's case of OSA, the higher the pressure used for therapy.
What is APAP?
Automatic positive airway pressure (APAP) relies on the same principles as CPAP. It's different because the machine is set differently, though the machine and setup look the same.
How does APAP work?
APAP's pressure settings are not limited to a single pressure, but to a range of pressures.
These machines are built to fluctuate within this range of pressures automatically when it delivers air. It depends on algorithms inside the machine which sense subtle breathing changes that take place throughout the night.
Who uses APAP?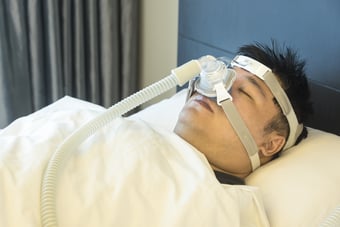
People who only experience apneas during REM sleep, or who prefer to sleep on their back, or who have allergies or congestion, can benefit from the "smart" features of this PAP device.
What is BiPAP?
BiPAP stands for bilevel positive airway pressure. It is also sometimes* referred to as BPAP or bilevel PAP. Like APAP, its uses and appearance are similar to CPAP, but its settings are different.
How does BiPAP work?
BPAP is set up to provide dual pressures: one for inhalation (IPAP) and another (lower) pressure for exhalation (EPAP). This therapy can also be set to match a person's breaths-per-minute rate or to sense a significant shift in their breathing and compensate for it by adjusting pressures so the person can maintain a steady pattern.
Who uses BiPAP?
Some people do not tolerate the single continuous pressure delivered in CPAP. Either the pressure itself is too high for them to adjust to, or they struggle to exhale against the incoming single pressure. BiPAP allows them to have a lighter EPAP pressure to make it easier to exhale.
Also, people with specific kinds of lung disorders (in example: chronic obstructive pulmonary disorder, or COPD) or congestive heart failure (CHF) may benefit from using bilevel PAP. People who experience c entral sleep apnea may also use BiPAP to good outcomes.
entral sleep apnea may also use BiPAP to good outcomes.
Central sleep apnea (CSA) occurs when the brain fails to signal to the lungs to breathe as you sleep.
What is ASV?
ASV stands for adaptive servo ventilation. It is the most sophisticated form of NIV and its use is reserved for specific kinds of patients.
Again, this machine may look very similar to all the other PAP machines out there, but it has unique settings and technology that set it apart.
How does ASV work?
ASV is typically the last line of defense in treating CSA. Patients usually start on BiPAP for this condition, but if this therapy doesn't work, they are switched to ASV. ASV machines are also used to treat patients who have been diagnosed with OSA, but who go on to develop patterns of CSA that bilevel PAP does not relieve.
Its algorithms are built to maintain not only consistent respiratory patterns, but healthy blood oxygen levels throughout the night. ASV not only adjusts to a multitude of breathing problems during sleep to help the user maintain consistency, it provides support for breathing so oxygen levels never dip below 90 percent and the user never has to struggle to maintain their respiratory rate.
Who uses ASV?
ASV machines are designed to treat CSA, mixed sleep apnea (a combination of obstructive and central respiratory events), and something known as Cheyne-Stokes respiration, in which abnormal breathing patterns take on a crescendo-decrescendo effect that results i n apnea.
n apnea.
NOTE: ASV is not used for specific kinds of heart failure patients, however. In particular, people with symptomatic chronic heart failure (identified as the cardiac category, NYHA 2-4) who experience a reduced left ventricular ejection fraction that is equal to or less than 45 percent should not use this therapy, as this can increase mortality risk.
Which therapy is best for me?
Your specific sleep breathing problems generally determine what form of NIV you will be prescribed:
-
For those with less severe or complicated problems with OSA, CPAP and APAP are common approaches
-
For those with more severe OSA, additional problems with CSA and other chronic health conditions, BiPAP and ASV may be the best choice
If you are unclear what type of machine you are using or whether you are using the correct therapy for your particular problem, don't hesitate to ask your physician to clarify which therapy is best for you. A DME provider is also skilled at checking your equipment for you in the event you need more information.
*Please note that BiPAP actually refers to the proprietary brand name of one manufacturer's bilevel PAP system, and not to all bilevel PAP in general. The term "BiPAP" has, regardless, come to be used universally to refer to all machines in this NIV category.











Leave a comment